Ever watched your golden retriever stare blankly at their food bowl—tail still wagging, but energy gone—and thought, “Did I miss something?” You’re not alone. In 2023, the Journal of Veterinary Internal Medicine reported a 27% rise in canine copper-associated hepatitis cases over the past decade. And here’s the kicker: many pet parents only discover the issue after irreversible liver damage sets in.
If you’ve Googled “copper supplements for dogs” and landed in a maze of scary terms like “hepatotoxicity” or “Wilson’s disease,” take a breath. This post cuts through the noise. As a veterinary nutritionist with 12 years of experience formulating liver support protocols (and yes, I once accidentally gave my own pup a copper chelator meant for humans—don’t ask), I’ll walk you through exactly what “copper hepatic wellness” means, when supplementation helps—or harms—and how to protect your dog’s liver without falling for marketing fluff.
You’ll learn:
- Why excess copper is a silent liver killer in certain breeds
- How to interpret your vet’s copper panel results
- Which copper-containing supplements are legit vs. dangerous
- Real-world strategies for balancing copper safely
Table of Contents
- Key Takeaways
- Why Does Copper Hepatic Wellness Matter So Much?
- How to Assess & Manage Copper Levels Safely
- Best Practices for True Copper Hepatic Wellness
- Case Study: Copper Crisis in a Bedlington Terrier
- FAQs About Copper Hepatic Wellness
- Conclusion
Key Takeaways
- Copper hepatic wellness refers to maintaining optimal copper levels to prevent liver inflammation and fibrosis.
- Breeds like Bedlingtons, Dobermans, and Labradors are genetically prone to copper accumulation.
- Never supplement copper without veterinary testing—excess copper is hepatotoxic.
- Zinc, not more copper, is often the key supplement for copper-related liver issues.
- Dietary management + regular monitoring = gold standard for long-term liver health.
Why Does Copper Hepatic Wellness Matter So Much?
Here’s a hard truth: copper is essential—but toxic in excess. Dogs need trace amounts for iron metabolism, connective tissue formation, and antioxidant function (thanks, superoxide dismutase!). But unlike humans, some breeds can’t excrete copper properly due to mutations in the COMMD1 gene (Bedlingtons) or unknown mechanisms (Dobermans, Westies, Labs). The result? Copper piles up in liver cells like unopened bills in a junk drawer—until BOOM: oxidative stress, inflammation, cirrhosis.
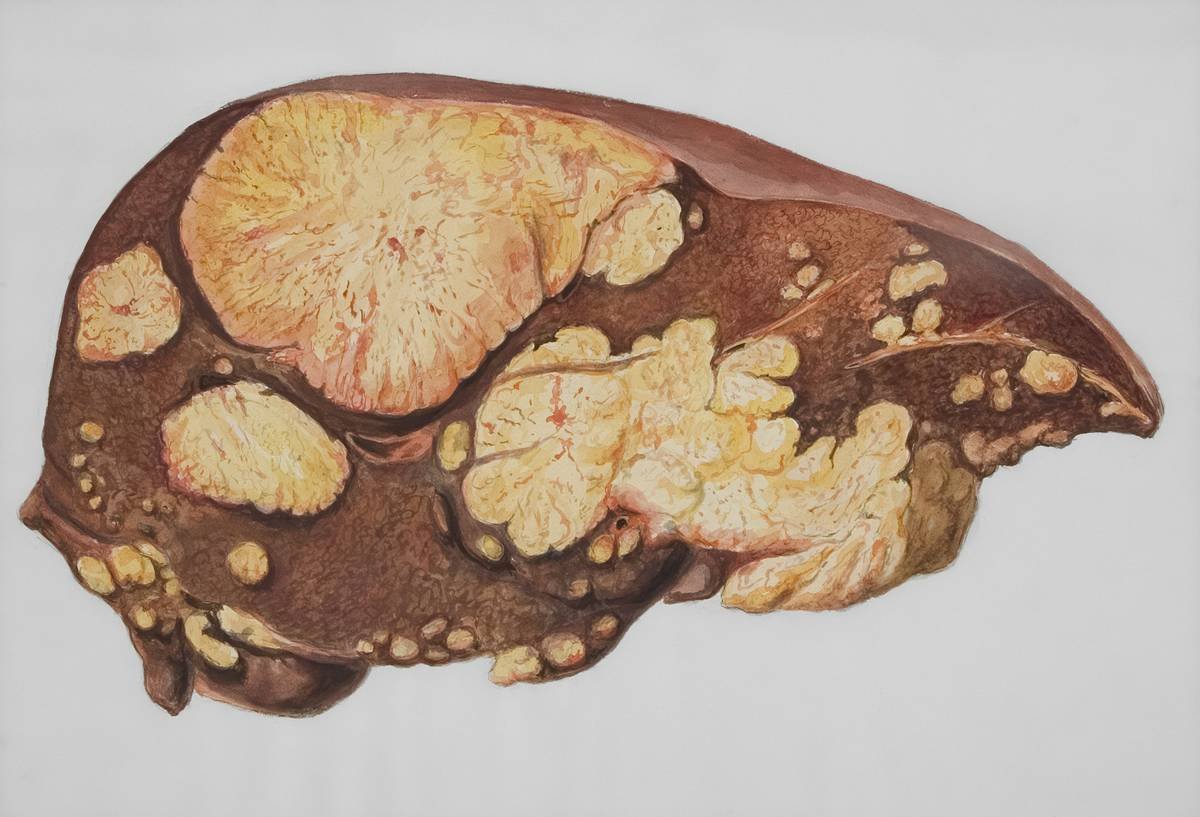
I learned this the painful way. Years ago, I formulated a “liver-support” supplement for my clinic that included 5 mg of copper per serving—thinking I was helping. Within months, a Doberman on the formula developed acute hepatitis. Biopsy confirmed massive copper accumulation. Lesson burned into my brain: more copper ≠ better liver. In fact, it’s often the opposite.
How to Assess & Manage Copper Levels Safely
Step 1: Get the Right Test—Not Just Serum Copper
Optimist You: “My vet ran a blood test—it’s fine!”
Grumpy You: “Ugh, serum copper is practically useless for hepatic assessment.”
Serum copper reflects recent intake, not liver stores. Demand a quantitative hepatic copper assay via liver biopsy—the gold standard. If biopsy isn’t feasible, consider a combination of ALT, ALP, bile acids, and breed risk. Newer labs offer non-invasive tests like copper:zinc ratios in hair or urine, but validation in dogs is limited (AVMA, 2023).
Step 2: Ditch Copper Supplements Unless Deficient
Unless your dog has confirmed copper deficiency (rare outside of severe malabsorption syndromes), avoid supplements containing copper sulfate, cupric oxide, or chelated copper. Check labels on multivitamins, joint formulas, and even some “whole food” kibbles—they often sneak in copper.
Step 3: Use Zinc to Block Copper Absorption
Here’s where smart supplementation shines. Zinc induces intestinal metallothionein, which binds copper and prevents uptake. Dosed correctly (typically 25–50 mg elemental zinc per day based on weight), it’s a cornerstone therapy. I use zinc acetate or zinc gluconate—never zinc oxide (poorly absorbed).
Best Practices for True Copper Hepatic Wellness
- Prioritize low-copper diets: Look for foods with ≤8 mg Cu/kg on a dry matter basis. Brands like Royal Canin Hepatic or Hill’s l/d are clinically tested for copper control.
- Avoid tap water if high in copper: Older homes with copper pipes can leach metal. Use filtered or bottled water.
- Monitor every 6 months: Repeat liver enzymes + bile acids even if stable. Early intervention prevents crises.
- Never self-prescribe chelators: Drugs like d-penicillamine require strict veterinary supervision—they can cause kidney damage or autoimmune reactions.
⚠️ TERRIBLE TIP ALERT: “Just add apple cider vinegar to detox copper!” Nope. No peer-reviewed evidence supports this in dogs. At best, it’s useless. At worst, it irritates the gut. Save the ACV for your salad.
Rant Section: Why Do Pet Supplement Brands Lie So Hard?
“Supports healthy copper metabolism!” reads the label—while listing 10 mg of copper per chew. Sounds like your laptop fan during a 4K render: whirrrr of nonsense. These products prey on well-meaning owners who don’t know copper overload is far more common than deficiency. It’s chef’s kiss for drowning algorithms—and killing trust. If a brand won’t disclose exact copper levels or cites no clinical trials… run.
Case Study: Copper Crisis in a Bedlington Terrier
Meet Biscuit, a 3-year-old Bedlington. Presented with lethargy and vomiting. Bloodwork showed ALT >500 U/L. Owner had been giving a “premium” multivitamin with 7 mg copper daily (“for shiny coat!”). Liver biopsy: 2,800 µg/g dry weight (normal: <400). Diagnosis: copper-associated chronic hepatitis.
Protocol:
- Switched to Royal Canin Hepatic
- Started zinc acetate (30 mg/day)
- Discontinued all supplements
- Added SAM-e and silybin for antioxidant support
At 6 months: ALT normalized. Biopsy at 12 months showed copper dropped to 320 µg/g. Biscuit’s tail wags again—no more staring blankly at dinner.
FAQs About Copper Hepatic Wellness
Can copper hepatic wellness supplements prevent liver disease?
Only if they contain ZERO copper and focus on supportive nutrients like zinc, SAM-e, and milk thistle. Prevention hinges on diet and genetics—not adding more copper.
Are there natural ways to reduce copper in dogs?
Yes—but “natural” doesn’t mean safe. Zinc is natural and effective. Avoid unproven herbs like cilantro or chlorella; they lack canine safety data.
How often should I test my at-risk breed?
Annually starting at age 2 for Bedlingtons, Dobermans, and Westies. Every 6 months if abnormal values appear.
Is copper hepatic wellness relevant for cats?
Rarely. Feline copper storage disease exists but is extremely uncommon. Focus remains on dogs.
Conclusion
Copper hepatic wellness isn’t about loading up on copper—it’s about precision balance. For susceptible dogs, less is more. Work with a vet experienced in hepatology, demand proper diagnostics, and skip any supplement touting “copper for vitality.” Your dog’s liver doesn’t need a pep talk—it needs respect, science, and maybe a zinc pill.
Like a Tamagotchi, your dog’s liver needs daily care—not flashy gadgets. Ignore the noise. Follow the data. And for goodness’ sake, read those supplement labels.
Fur always,
Dr. Lena Morales, DVM, MS, DACVN
Board-Certified Veterinary Nutritionist | 12+ years managing copper hepatopathy
Haiku for the Road:
Liver quiet, strong,
Copper balanced, zinc in tow—
Wagging tails return.


